The Situation
A manufacturer with over 4,700 members in the Western United States was unhappy with their pharmacy arrangement and needed more expertise to help curb spend. Their plan was not protecting them from rising spend and high-dollar claims, and they did not have the support they needed from their PBM. The company needed a new pharmacy benefits partner who was an expert in the space and willing to look at their plan with a critical eye.
4,700
Members
The Solution
The manufacturer partnered with RxBenefits to conduct an in-depth analysis of their contract and plan design. Our expert clinical pharmacists provided a free Pharmacy Performance Analysis and identified specific risk areas to minimize costs. They then suggested a tailored clinical and plan design strategy to maximize savings, which included:
Narrowing the Formulary
Offers better pricing and additional oversight on covered medications to maximize the use of plan dollars with limited member disruption.
Low Clinical Value Formulary Exclusions
Prevents unnecessary drug spend by removing non-essential, high-cost, low clinical value medications from the formulary.
Our clinical team continually monitored drugs in the market and updated the low clinical value drug list throughout the year, which produced additional value.
High Dollar Claim Review
Provides umbrella protection against unnecessary spending on high-cost medications by providing an independent pharmacist review of claims greater than $1,000.
Our clinical team provided additional oversight through prior authorization reviews for certain high-cost prescription drug claims, giving the organization insight into the specific drugs contributing to its monthly plan cost and limiting its exposure.
The Impact
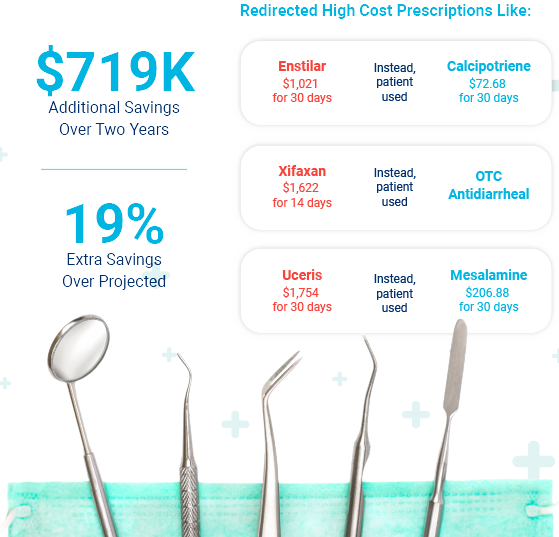
The client achieved $719k in savings in plan cost – 19% more than projected – over a two-year period by implementing plan design changes and clinical optimization solutions recommended by RxBenefits. The company was able to ensure its pharmacy dollars paid for the most clinically appropriate and cost-effective therapies, which created more value for its employees – all with minimal disruption.
Originally published: April 8, 2021 | Updated on: April 22, 2024
